Sign up to our newsletter!
White Coat Hypertension Is No Longer Benign. See Why It Matters Here.
White coat hypertension (WCH) is a condition where your blood pressure reading is high in your doctor's or healthcare provider's office, but normal at home or outside their office. It is now believed that this condition should be taken seriously. See what you can do here.
 Nurse trying to calm down patient with white coat hypertension.
Nurse trying to calm down patient with white coat hypertension.Have you ever gone to see your doctor and have your blood pressure measured, only for the doctor to says: hey, your blood pressure is too high?
You then went home, or to your local pharmacy, took your blood pressure reading and it was normal?
If this happens repeatedly, then you have a condition called white coat hypertension.
White coat hypertension is a component of white coat syndrome, which consists white coat effect, mask hypertension and white coat hypertension.
What Causes This Type of Hypertension
White coat hypertension is believed to be caused by an abnormal response of the nervous system.
Research is suggesting that it is not caused by anxiety alone.
Many people do not "like doctors" and when they go in to their healthcare provider's office, they may become preoccupied with what might be discovered during an examination and this triggers the abnormal response that brings about white coat syndrome or hypertension.
What Is A Normal Blood Pressure Reading?
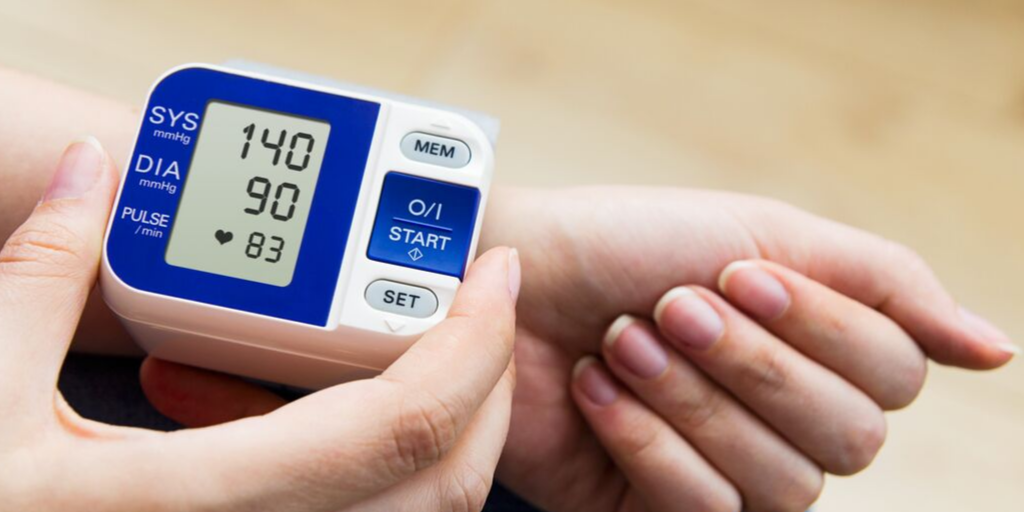 Blood pressure readings from 140/90 mmHg is abnormal. If this persists, it is referred to as hypertension.
Blood pressure readings from 140/90 mmHg is abnormal. If this persists, it is referred to as hypertension.A normal blood pressure is anything between 90/60 mmHg and 130/80 mmHg.
Elevated blood pressure (now referred to as mild hypertension) is a blood pressure reading between 130/80 mmHg and 140/90 mmHg.
Hypertension ( or grade 2 hypertension, as per the 2017 American College of Cardiology guideline) is blood pressure readings of 140/90 mmHg.
Note that no person's blood pressure reading stays the same all the time. Our emotion, stress level, or activity or lack of, foods and drinks (like coffee consumption and smoking), affects our blood pressure reading.
It is also important to note that your blood pressure readings at your healthcare provider's office is usually 10/5 mmHg higher than what you tae at home. This is normal, and not considered white coat hypertension.
If your blood pressure readings goes higher than 140/90 mmHg repeatedly when it is measured by a healthcare provider, but is goes back to below 130/80 mmHg outside their office, then you have white coat hypertension.
Diagnosis
White coat hypertension is diagnosed by one of three ways:
Home Blood Pressure Reading.
Your doctor may ask you to buy a blood pressure monitor if you do not already have one.
You will then need to record your blood pressure two times daily for seven days - preferably once in the morning and once in the evening.
These are best done when you are most relaxed. The readings are then looked at and if your blood pressure readings are consistently lower than the readings obtained in the consulting room, then a diagnosis of white coat hypertension can be made.
Mental Arithmetic.
A study published in the American Journal of Hypertension showed that patients who were suspected to have white coat hypertension and asked to do mental arithmetic, once they focused on the mental math, their blood pressure dropped.
This was used as a quick way to screen for possible WCH.
Ambulatory Blood Pressure Monitoring.
This is perhaps the most reliable way to make a diagnosis of white coat syndrome.
Ambulatory blood pressure monitoring is done by having a telemedicine blood pressure monitor attached to your arm over a 24 to 48 hours period.
The machine then takes your blood pressure readings every 15 minutes or so and have the result sent to a computer database.
Your blood pressure readings over that time - during your wake hours and during your sleep is then studied and your average blood pressure over this time computed.
If the result shows a blood pressure reading that is consistently below 140/90 mmHg, then you are considered non-hypertensive.
Why A Diagnosis of White Coat Hypertension Matters
You may End Up Receiving Unnecessary Treatment Without A Diagnosis of WCH.
It is very important to be able to determine if you have white coat hypertension or not.
This is because if each time you go into your doctor's or healthcare provider's office and your blood pressure is high, and they do not realise that you suffer with white coat hypertension, you could end up being treated with blood pressure pills unnecessarily.
You could then develop complications - like lightheadedness, dizziness, and even instability and falls because the medication could make your blood pressure too low.
You may also suffer from the specific side effects of the medication used in treating you, without any trade-off benefit.
So it is important that a diagnosis of white coat hypertension is made or excluded before you get treatment for a new diagnosis of hypertension.
White Coat Hypertension Is No Longer Considered Benign.
For many years, doctors thought that having white coat hypertension is benign and does not require any intervention.
With improved understanding of human physiology, it has now been established that WCH correlates very well with your Heart Rate Variability index, which can help predict those who would come down with heart disease.
So, the new understanding is that those with significant white coat hypertension are more likely to hypertension and other heart related disease.
The advice now that if you have WCH, seek treatment.
Treatment of White Coat Hypertension

Because WCH is considered an early predictor of the development of hypertension, stroke and heart disease, the new recommendation is that this condition should be treated or given attention to when found in a patient.
All the leading experts, including the American College of Cardiologists do not endorse the use of medications to treat white coat hypertension.
The treatment of white coat hypertension involves lifestyle modifications. This will include mindfulness, getting good sleep, exercise and nutrition.
If you drink more than moderate alcohol or smoke, stopping these habits would also be helpful.
If you are diagnosed with white coat hypertension, have your blood pressure checked regularly at home and keep records. Any persistent elevation of your home blood pressure readings should be discussed with your doctor.
In Summary
White coat hypertension is a very common condition. It is seen as the very early stage in a continuum or spectrum of disease that ends as hypertension.
It is important to make a firm diagnosis of this condition so as to avoid unnecessary treatment with medications.
Treatment is mainly behavioural and lifestyle modifications.
Everyone with a diagnosis of white coat hypertension should ensure they take their blood pressure readings regularly so that they do not then go on to develop hypertension without knowing.